From Decline to Momentum: Inside a Leadership Turnaround at a Busy Health Center in Ethiopia
By Merian Abdirkadir, Amina Kanpise, Bruktawit Lema, Dedefo Teshite, Dr. Fetya Abbagidi, Dr. Hana Gebregzabher, and Betel Sahile, EngenderHealth Ethiopia
Every day, dozens of women arrive at Nifas Silk Woreda 2 Health Center in Addis Ababa, Ethiopia, to give birth, seek postnatal care, or bring their infants for immunizations. As one of the city’s busiest public health facilities, the center plays a critical role in protecting the health of mothers and newborns.
But in early 2025, something wasn’t working.
Despite having trained staff, essential supplies, and technical support through EngenderHealth’s Integrated RMNCH+PPFP Scale-Up Project, the number of women receiving Immediate Postpartum Family Planning (IPPFP) was going down instead of up.
By June 2025, IPPFP uptake had fallen from 24% to just 18%.
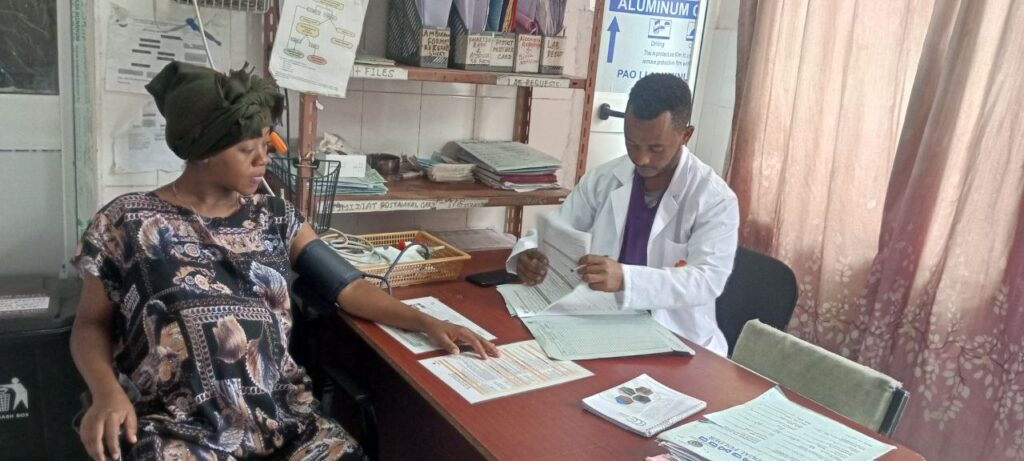
For a facility serving dozens of births each month, this decline meant missed opportunities: women were leaving without counseling, without options, and without the ability to safely space future pregnancies. Behind the numbers were mothers and newborns facing preventable risks.
Something had to change.
“What Is Stopping Us from Giving Every Woman the Care She Deserves?”
In July 2025, Health Center Director Mr. Robel Tesema brought together his team— midwives, the medical director, Family Health Teams, and EngenderHealth partners— for an honest conversation about what was happening inside the facility.
He asked a simple but profound question: “What is stopping us from giving every woman the care she deserves?”
The discussion revealed challenges many busy facilities face. Providers were stretched thin, accountability was unclear, and family planning counseling wasn’t consistently integrated across services. Data was collected but rarely reviewed or used to drive decisions. Teams worked in silos, leadership engagement in Reproductive, Maternal, Newborn, and Child Health (RMNCH) service utilization follow-up was limited, and mothers were frequently missed in postnatal visits, immunization appointments, and community outreach.
Rather than discouraging the staff, the conversation created something new: shared ownership of the problem and a solution.
Turning Insight Into Action Through Leadership and Teamwork
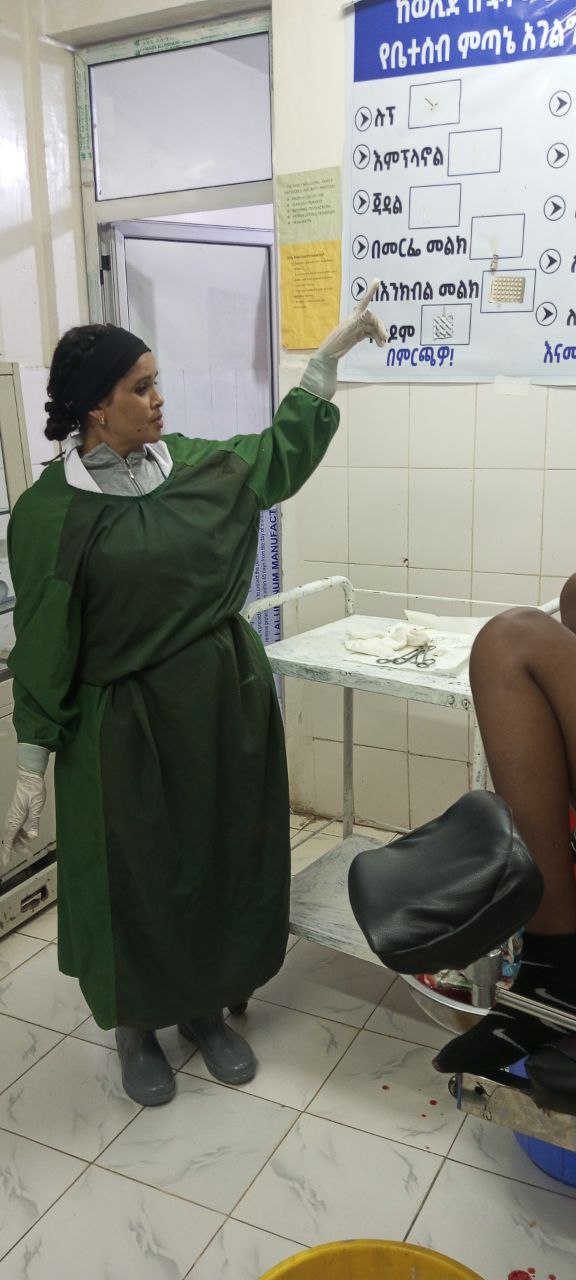
What followed was not a complicated overhaul, but a series of practical, leadership-driven changes designed to reconnect teams, strengthen accountability, and make data visible and useful.
Daily performance updates shared through a Telegram group helped staff stay informed and motivated. IPPFP indicators were added to a real-time dashboard so progress and gaps were clear to everyone. Weekly review meetings ensured data was actively used, not just recorded.
The EngenderHealth Family Health Teams expanded counseling beyond the facility, reaching women in their homes who had previously been missed. A client feedback logbook gave women a voice and helped providers improve the quality and respectfulness of care.
Strong performance was recognized and celebrated, reinforcing a culture of shared responsibility. Recognition of strong staff performance boosted morale and accountability, reinforcing a culture of shared accountability.
Individually, these steps were small. Together, they were transformative.
A Remarkable Turnaround in Just Three Months
By October 2025, the transformation was undeniable.
IPPFP uptake soared from 18% to 73%—a more than fourfold increase and one of the fastest improvements seen in the project. Coordination improved, and family planning counseling became routine across antenatal care, postnatal care, immunization services, under-five clinics, and community outreach.
Most importantly, women noticed the difference.
One mother wrote in the feedback logbook: “They took their time to explain every method. I felt respected.”
Another shared: “I was given privacy, and my worries were heard. Thank you.”
Trust grew. And with it, service uptake increased.
Why This Success Matters
This story is about more than just percentages. It’s about mothers leaving the facility informed, respected, and confident in their choices. With increased IPPFP uptake, women are better able to space pregnancies, reduce health risks, and protect their newborns. Providers are better positioned to prevent complications like postpartum hemorrhage. And reproductive health services are now integrated seamlessly across the continuum of care.
The experience at Nifas Silk Woreda 2 Health Center shows what’s possible when leadership, data, teamwork, and community engagement align. Rapid, sustainable improvements don’t always require new resources: they require commitment, clarity, and coordination.
Building a Model for Sustainable Change
The practices that fueled this turnaround are now part of the health center’s routine operations. Leadership-led monitoring ensures accountability. Integrated counseling across all service points ensures no woman is missed. Daily communication keeps teams aligned, while community follow-up strengthens continuity of care beyond the facility walls.
These lessons aren’t staying in one place. The model is being shared with other facilities in Addis Ababa and beyond, offering a replicable path toward stronger health systems.
A Story of Hope and Possibility
The story of Nifas Silk Woreda 2 Health Center shows what happens when health workers are empowered with the right tools and support, and when leaders step forward to ask hard questions and act on the answers.
It’s a story of change and possibility. It shows how, over a period of three months, the health center began to change—moving from decline to steady momentum, from missed opportunities to more respectful, integrated care, and from 18% to 72.6% uptake in immediate postpartum family planning.
Most importantly, it is a story about mothers. Mothers who now leave the facility with the information and choices they deserve—healthier, safer, and more confident about the future.
