Closing the Gap: Women Leading Change through Early Counseling at Gelan Health Center in Ethiopia

By Merian Abdirkadir, Amina Kanpise, Bruktawit Lemma, Betel Sahile, and Yanet Ayenachew, EngenderHealth Ethiopia
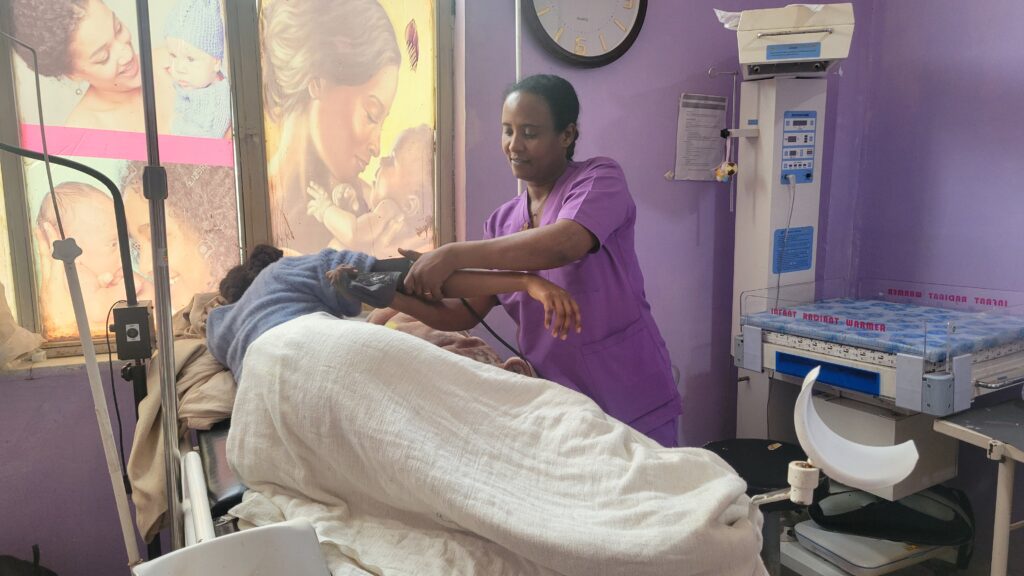
In the bustling antenatal care (ANC) room at Gelan Health Center in Addis Ababa, Ethiopia, mornings are filled with pregnant women waiting for checkups, ultrasound referrals, and reassurance that their babies are healthy. For many, their pregnancies were planned. For others, they were not. Almost all share the same concern: how to protect their health during delivery and after childbirth while caring for a newborn.
Hearing Women Before Delivery
Midwives at Gelan recall women returning for their six-week postnatal visits already pregnant again—confused, overwhelmed, and sometimes seeking comprehensive abortion care.
Family planning conversations traditionally happened after delivery, when women were exhausted and unsure of their options.
“We realized we were speaking to women when it was already too late,” explains Tigist Lemma, a BSc midwife at the facility. “They needed this information earlier—when they still had time to think, discuss with their families, and prepare.”

Early Conversations, Informed Choices
With support from EngenderHealth’s RMNCH+PPFP project, Gelan Health Center began integrating immediate postpartum family planning (IPPFP) counseling directly into ANC visits.
Now, while checking blood pressure or measuring fundal height, midwives initiate structured, client-centered conversations about postpartum contraception. They explain available methods, discuss timing, address concerns, and record each woman’s preferences and readiness.
“When we talk during ANC, women are calmer and more focused,” Tigist says. “They ask questions. They involve their partners. They come to delivery already knowing what they want.”
Confidence Before Labor
Providers report that women now enter the labor ward with clearer intentions about postpartum contraception. Acceptance of IPPFP has increased, and midwives are seeing fewer unintended pregnancies and fewer abortion-related visits linked to missed counseling opportunities.
Documentation has also improved. Counseling sessions, chosen methods, and follow-up plans are systematically recorded to ensure continuity of care and accountability.
“Before, it depended on memory,” Tigist reflects. “Now, we follow the woman’s journey from ANC to delivery.”

Tools that Save Lives
The improvements at Gelan extend beyond counseling. While providers are helping women plan for healthy spacing after childbirth, they are also strengthening the care women receive during delivery itself.
At the health center, providers are introducing the E-MOTIVE bundle of care to respond quickly to postpartum hemorrhage, the leading cause of maternal death worldwide. Postpartum hemorrhage—severe bleeding after birth—can become life-threatening within minutes if it is not detected and treated quickly.
In the delivery ward, blood-collection drapes now replace visual estimates of blood loss, allowing providers to measure bleeding accurately and recognize complications earlier. When excessive bleeding is detected, providers immediately begin a coordinated treatment bundle that may include uterine massage, medicines that help the uterus contract, intravenous fluids, clinical examination, and referral for advanced care when needed.
Together, these improvements help ensure women receive safer care throughout the childbirth journey.
At its heart, Gelan Health Center’s transformation is about timing and trust. By moving family planning counseling earlier in the pregnancy journey, providers give women space to think, discuss, and decide. They are replacing rushed postpartum conversations with clear, well-informed preparation. They are turning missed opportunities into informed choices.
“We are not just providing services,” Tigist says. “We are helping women plan their futures.”
At Gelan Health Center, that future begins long before delivery and continues with every informed decision a woman makes for herself and her family.
